Early SPECT/CT imaging can identify advanced prostate cancer patients most likely to survive long term after lutetium-177 (Lu-177) prostate-specific membrane antigen (PSMA)-617 therapy, according to a study published April 28 in Radiology.
The finding is from a secondary analysis of 74 participants in the ENZA-p trial in Australia, with Lu-177 PSMA-617 SPECT/CT total tumor volume (TTV) complete response (CR) at six weeks associated with overall survival, noted lead author Narjess Ayati, MD, of St Vincent’s Hospital Sydney, and colleagues.
“This finding suggests that early TTV CR at SPECT/CT could serve as an alternative to interim PSMA PET/CT-derived CR for guiding adaptive dosing and deintensification treatment regimens for PSMA radioligand therapy,” the group wrote.
The ENZA-p trial previously demonstrated improved overall survival (OS) and quality of life in patients with metastatic castration-resistant prostate cancer (mCRPC) who received Lu-177 PSMA-617 in combination with enzalutamide, compared with enzalutamide alone. The primary trial used a PSMA PET/CT scan at 12 weeks to determine whether patients received two or four total doses of Lu-177 PSMA-617. SPECT/CT was performed 24 hours after each injection as an exploratory endpoint, the authors explained.
In this secondary analysis, the group analyzed SPECT/CT data from 74 men who received enzalutamide plus Lu-177 PSMA-617 and had scans at both baseline and six weeks. The team measured TTV and mean standardized uptake value (SUVmean) at each time point and assessed whether early imaging response predicted OS.
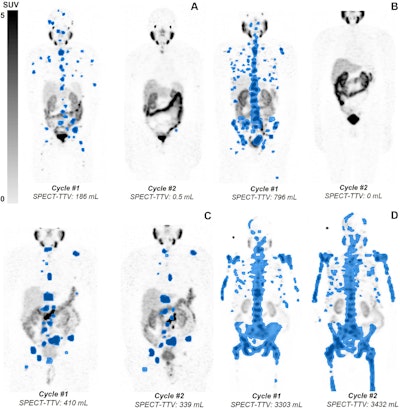
 Quantification of total tumor volume (TTV) at lutetium-177 prostate-specific membrane antigen (PSMA)–617 SPECT/CT shows heterogeneous TTV responses between dose 1 (Cycle #1) and dose 2 (Cycle #2) in participants with metastatic castration-resistant prostate cancer. Posttherapy coronal attenuation-corrected noncontrast SPECT/CT maximum intensity projection images demonstrate (A) near-complete response in a 76-year-old man, (B) complete response in an 83-year-old man, (C) partial TTV reduction (not complete response) in a 69-year-old man, and (D) TTV increase (i.e. progressive disease) in a 74-year-old man. Blue-shaded regions represent semiautomatically segmented PSMA-avid tumor volume, with associated TTV values given at the bottom of each panel. The gradient bar shows standardized uptake value (SUV) from 0 to 5.RSNAKey findings included the following:
Quantification of total tumor volume (TTV) at lutetium-177 prostate-specific membrane antigen (PSMA)–617 SPECT/CT shows heterogeneous TTV responses between dose 1 (Cycle #1) and dose 2 (Cycle #2) in participants with metastatic castration-resistant prostate cancer. Posttherapy coronal attenuation-corrected noncontrast SPECT/CT maximum intensity projection images demonstrate (A) near-complete response in a 76-year-old man, (B) complete response in an 83-year-old man, (C) partial TTV reduction (not complete response) in a 69-year-old man, and (D) TTV increase (i.e. progressive disease) in a 74-year-old man. Blue-shaded regions represent semiautomatically segmented PSMA-avid tumor volume, with associated TTV values given at the bottom of each panel. The gradient bar shows standardized uptake value (SUV) from 0 to 5.RSNAKey findings included the following:
At six weeks, the median change in TTV based on SPECT/CT was −57%, with 61% (45 of 74) of participants showing a 50% or greater reduction in TTV.
The two-year survival rate with TTV complete response was 83%, versus 67% without TTV complete response (hazard ratio, 0.26; log-rank p = 0.02).
The two-year survival rate was 76% with a deep prostate-specific antigen (PSA) response but not TTV complete response, and 54% if neither a deep PSA response nor TTV complete response was observed.
Compared with interim PSMA PET/CT at 12 weeks, six-week SPECT/CT offers earlier actionable data, requires no additional radiopharmaceutical administration, and is more broadly accessible, the authors noted.
“This approach may support treatment personalization with greater convenience and lower cost as an alternative to interim PSMA PET/CT imaging,” the group concluded.
In an accompanying editorial, Samuel Galgano, MD, and Eric Turner, MD, both of the University of Alabama at Birmingham, wrote that the study is important for the future of Lu-177 PSMA-617 post-therapy imaging in that it provides a compelling argument to increase its overall use in general clinical practice and to go beyond the typical qualitative evaluation.
“With volumetric analysis, there can be greater diagnostic confidence that some patients with early treatment responses may be able to receive fewer than six doses at time of initial therapy, thus reducing overall toxicities as well as decreasing health care costs,” the pair wrote.
In the future, as the number of radioligand therapies increases and quantitative software continues to improve, clinicians need to be aware of this information to best evaluate their patients from both a prognostic and treatment response perspective, Galgano and Turner concluded.
The full study is available here.
Whether you are a professional looking for a new job or a representative of an organization who needs workforce solutions - we are here to help.